Drexel Hill (484) 521-0233
West Chester (610) 436-5883

Drexel Hill (484) 521-0233
West Chester (610) 436-5883


Diabetic neuropathy is a serious complication of diabetes that results from nerve damage caused by prolonged high blood sugar and elevated blood fats. This condition often targets the nerves in the lower legs and feet, leading to what is known as peripheral neuropathy. Studies show that between one-third and one-half of people with diabetes will experience this condition. Diabetic neuropathy can bring on a range of uncomfortable symptoms, including numbness and weakness, burning, tingling, and pain in the lower limbs. Additionally, the diminished sensation can make you more susceptible to unnoticed wounds on your feet, which increases the risk of infections and complications. To manage diabetic neuropathy effectively, it is suggested you schedule an appointment with a podiatrist, ensuring that any potential issues are caught early and treated appropriately.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with the podiatrists from Dr. Siegerman & Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Neuropathy is a condition in which the nerves in the body become damaged from a number of different illnesses. Nerves from any part of the body, including the foot, can be damaged. There are several forms of neuropathy including peripheral neuropathy, cranial neuropathy, focal neuropathy, and autonomic neuropathy. Furthermore there is also mononeuropathy and polyneuropathy. Mononeuropathies affect one nerve while polyneuropathies affect several nerves. Causes of neuropathy include physical injury, diseases, cancers, infections, diabetes, toxic substances, and disorders. It is peripheral neuropathy that affects the feet.
The symptoms of neuropathy vary greatly and can be minor such as numbness, sensation loss, prickling, and tingling sensations. More painful symptoms include throbbing, burning, freezing, and sharp pains. The most severe symptoms can be muscle weakness/paralysis, problems with coordination, and falling.
Podiatrists rely upon a full medical history and a neurological examination to diagnose peripheral neuropathy in the foot. More tests that may be used include nerve function tests to test nerve damage, blood tests to detect diabetes or vitamin deficiencies. Imaging tests, such as CT or MRI scans, might be used to look for abnormalities, and finally nerve or skin biopsies could also be taken.
Treatment depends upon the causes of neuropathy. If the neuropathy was caused by vitamin deficiency, diabetes, infection, or toxic substances, addressing those conditions can lead to the nerve healing and sensation returning to the area. However if the nerve has died, then sensation may never come back to the area. Pain medication may be prescribed for less serious symptoms. Topical creams may also be tried to bring back sensation. Electrical nerve stimulation may be used for a period of time to stimulate nerves. Physical therapy can strengthen muscle and improve movement. Finally surgery might be necessary if pressure on the nerve is causing the neuropathy.
If you are experiencing sensation loss, numbness, tingling, or burning sensations in your feet, you may be experiencing neuropathy. Be sure to talk to a podiatrist to be diagnosed right away.
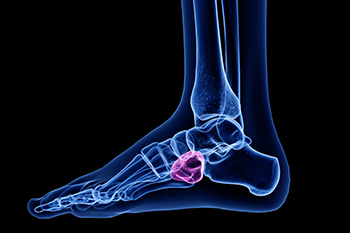
Cuboid syndrome, a condition affecting the foot, involves the cuboid bone, one of the seven tarsal bones located on the outer side of the foot. Positioned between the heel bone, which is also known as the calcaneus, and the 4th and 5th metatarsal bones, the cuboid bone plays a vital role in maintaining the arch of the foot and facilitating movement. This syndrome typically arises due to repetitive stress or trauma, such as overuse injuries common in athletes or sudden twists of the foot. The exact cause often involves the displacement, or subluxation, of the cuboid bone, leading to pain and discomfort on the outer edge of the foot, sometimes radiating into the toes. Symptoms may include swelling, tenderness, and difficulty bearing weight on the affected foot. If you have pain in this part of your foot, it is suggested that you visit a podiatrist who can provide an accurate diagnosis and treatment.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with the podiatrists from Dr. Siegerman & Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Cuboid syndrome mostly affects athletes, although it can affect non-athletes too. It is also known as cuboid subluxation or cuboid fault syndrome. This condition occurs when joints and ligaments near the cuboid bone of the foot are damaged, or when the cuboid bone itself is dislodged from its natural position. It is usually marked by pain on the outer side of the foot, which may be persistent or may come and go. Cuboid syndrome can be difficult to diagnose unless it becomes severe and more noticeable. Your doctor will likely ask questions about when the pain began and how long it has been present, and will put pressure on the cuboid bone to determine if that area is the origin of the pain.
Causes of Cuboid Syndrome
Disagreements Amongst Podiatrists Regarding Cuboid Syndrome
It is very important that when you experience any kind of pain on the side of your foot, you should seek medical care right away. If a subluxed cuboid is caught early, your feet may respond well to the treatment, and you can get back into sports or other activities again as soon as the pain subsides.

Peripheral artery disease, or PAD, affects blood circulation, often manifesting through symptoms related to the feet. Common signs include cramping, pain, or numbness in the feet during physical activity, which subsides with rest. Coldness or discoloration of the feet or toes, particularly in comparison to the unaffected leg, may also occur due to reduced blood flow. Slow-healing wounds or sores on the feet are another indicator, as PAD limits the delivery of oxygen and nutrients essential for tissue repair. PAD, caused by narrowed arteries due to plaque buildup, increases the risk of complications, such as infections and tissue death in severe cases. Regular foot exams from a podiatrist are essential for managing PAD. If you have symptoms of PAD, it is suggested that you are under the care of this type of doctor who can help you to manage this condition.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with the podiatrists from Dr. Siegerman & Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
 The human foot is a complex structure of bones, joints, muscles, tendons, and ligaments. It carries the body’s weight and enables upright walking, providing stability and flexibility. However, foot deformities can arise from various factors such as external pressures, certain foot postures, or underlying medical conditions. While some deformities are present at birth, others develop over time and can lead to significant discomfort and mobility issues. Splayfoot occurs when the metatarsal bones spread out, which causes the front of the foot to widen and can lead to pain and calluses. Fallen arches, or flat feet, result in the entire sole touching the ground due to weak foot muscles or wearing unsuitable footwear and causing long-term discomfort. Pronated feet, where the heel leans inward, often develop in overweight individuals or those with knock-knees. This may also lead to pain in the knees, hips, and back. High-arched feet place excessive pressure on the ball of the foot, increasing the risk of ankle injuries. If you are experiencing pain resulting from a foot deformity, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
The human foot is a complex structure of bones, joints, muscles, tendons, and ligaments. It carries the body’s weight and enables upright walking, providing stability and flexibility. However, foot deformities can arise from various factors such as external pressures, certain foot postures, or underlying medical conditions. While some deformities are present at birth, others develop over time and can lead to significant discomfort and mobility issues. Splayfoot occurs when the metatarsal bones spread out, which causes the front of the foot to widen and can lead to pain and calluses. Fallen arches, or flat feet, result in the entire sole touching the ground due to weak foot muscles or wearing unsuitable footwear and causing long-term discomfort. Pronated feet, where the heel leans inward, often develop in overweight individuals or those with knock-knees. This may also lead to pain in the knees, hips, and back. High-arched feet place excessive pressure on the ball of the foot, increasing the risk of ankle injuries. If you are experiencing pain resulting from a foot deformity, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
If you have any concerns about your feet, contact the podiatrists from Dr. Siegerman & Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Podiatry is a branch of medicine that deals with the study, diagnosis, and treatment of foot and ankle conditions. There are various subdivisions in podiatry; biomechanics is one of them. Biomechanics is the way in which the bones, muscles, and joints of the feet and lower limb interact with each other.
Our feet play crucial roles in the way we move, and it is rare to have feet that are completely symmetrical. Common biomechanical issues include high or low arches or uneven leg heights. Excessive pronation often leads to fallen arches, or flat feet, and is a common cause of running injuries. People whose feet are over-pronated tend to have flexible and unstable feet. Pain is usually experienced during walking and running.
At times, people may be able to adapt to these abnormalities without any difficulties, but in other cases, these issues can cause a great deal of pain. This pain occurs because the joints, muscles, ligaments, and tendons are put under an excess amount of stress during movement. Common symptoms of biomechanical problems stemming from the feet include hip pain, knee pain, leg cramps, ankle pain, lower back pain, weak ankles, tripping, heel pain, Achilles pain, and shin splints.
Many biomechanical issues can be treated with orthotics. Orthotics are shoe insoles that are used to help control the way the foot operates. They can provide relief from foot pain, heel pain, and knee pain. Depending on your specific case, you may need to purchase over-the-counter orthotics or custom orthotics to fit your feet. Your podiatrist will be able to prescribe the perfect orthotic for your feet to help you walk around with ease.
Gait is defined as the way we move our bodies from one point to another. This is usually done by either walking or running. Gait analysis is a method used to assess the way we walk or run to highlight biomechanical abnormalities. Gait analyses are a great way to take a detailed look at how you walk and how your foot moves while you walk. An examination of the feet will help your podiatrist understand why you are suffering pain in other parts of your body.

Foot ulcers are open wounds that develop on the feet, often affecting individuals with diabetes or impaired circulation. They typically occur due to a combination of factors, including neuropathy, which is nerve damage, poor blood flow, and pressure from footwear. Foot ulcers can vary in severity, from shallow sores to deep craters, and if left untreated, they can lead to serious complications such as infection and possibly amputation. The primary cause of foot ulcers is prolonged pressure or friction on the skin, which can result from wearing ill-fitting shoes, walking barefoot, or excessive rubbing. In diabetic individuals, high blood sugar levels can further exacerbate the risk by damaging nerves and blood vessels, impairing the body's ability to heal. Other contributing factors may include poor hygiene, smoking, obesity, and a history of foot problems. Recognizing the signs of a foot ulcer, such as redness, swelling, or drainage, is vital for prompt treatment and prevention of complications. If you have a foot wound, it is strongly suggested that you consult a podiatrist who can diagnose its severity, and offer treatment options that are right for you.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with the podiatrists from Dr. Siegerman & Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Request a free copy of
Laser Away Foot Pain!
today.