Drexel Hill (484) 521-0233
West Chester (610) 436-5883

Drexel Hill (484) 521-0233
West Chester (610) 436-5883

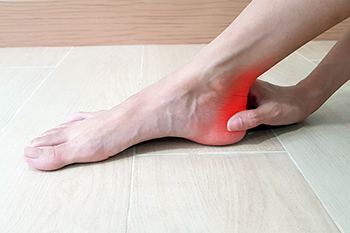 A heel spur is a painful bone growth on the heel. An Achilles heel spur is a bone spur on the back of the heel. This condition develops from the tugging of the heel bone due to a tight Achilles tendon. It can result from calf muscles that are not stretched properly, excess weight, shoes that stress the foot (such as high heels) – anything that strains the foot bone and allows calcium deposits to build. The spur can present as pain at the back of the heel, particularly intense after prolonged periods of rest. Walking, running, and lifting heavy objects can aggravate this condition. Patients who are struggling with heel pain that may be a heel spur should see a qualified podiatrist when this or any unusual symptoms of the feet occur.
A heel spur is a painful bone growth on the heel. An Achilles heel spur is a bone spur on the back of the heel. This condition develops from the tugging of the heel bone due to a tight Achilles tendon. It can result from calf muscles that are not stretched properly, excess weight, shoes that stress the foot (such as high heels) – anything that strains the foot bone and allows calcium deposits to build. The spur can present as pain at the back of the heel, particularly intense after prolonged periods of rest. Walking, running, and lifting heavy objects can aggravate this condition. Patients who are struggling with heel pain that may be a heel spur should see a qualified podiatrist when this or any unusual symptoms of the feet occur.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact the podiatrists from Dr. Siegerman & Associates. Our doctors will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the latest in diagnostic and treatment technology to meet your needs.
Heel spurs are the result of calcium deposits that cause bony protrusions on the underside of the heel. Heel spurs are usually painless, but they have the potential to cause heel pain. Heel spurs tend to be associated with plantar fasciitis, which is a condition that causes inflammation of the band of connective tissue that runs along the bottom of the foot. They most often occur to athletes whose sports involve a lot of running and jumping.
Some risk factors for developing heel spurs include running and jogging on hard surfaces, being obese, wearing poorly fitting shoes, or having walking gait abnormalities.
It is possible to have a heel spur without showing signs of any symptoms. However, if inflammation develops at the point of the spur’s formation, you may have pain while walking or running. In terms of diagnosis, sometimes all a doctor needs to know is that the patient is experiencing a sharp pain localized to the heel to diagnose a heel spur. Other times, an x-ray may be needed to confirm the presence of a heel spur.
Heel spurs can be prevented by wearing well-fitting shoes that have shock-absorbent soles. You should also be sure that you are choosing the right shoe for the activity you want to partake in; for example, do not wear walking shoes when you want to go on a run. Additionally, maintaining a healthy weight can be beneficial toward preventing heel spurs, as it will prevent an excess amount of pressure being placed on the ligaments.
There are a variety of treatment options for people with heel spurs. Some of these include stretching exercises, physical therapy, shoe inserts, or taping and strapping to rest stressed muscles and tendons. If you have heel pain that lasts longer than a month, don’t hesitate to seek help from a podiatrist. Your doctor can help you determine which treatment option is best for you.
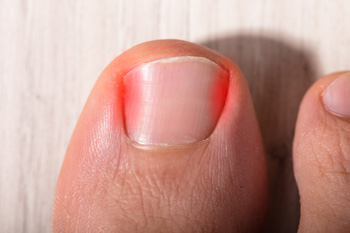 An ingrown toenail occurs when the outer edge of a toenail grows into the surrounding skin, rather than over it. This causes redness, swelling, pain, and inflammation around the ingrown toenail. The area is also at an increased risk of infection. Several factors make an ingrown toenail more likely to develop. Trimming the toenails improperly, by cutting them too short or into a rounded shape, makes the skin more likely to fold over the nail. Wearing shoes that are too tight or narrow in the toe area can squish the nails into the skin. Having excessively sweaty feet can make the skin surrounding the nails too soft, allowing the nail to pierce through the skin more easily. Sometimes an injury to the toenail can cause an ingrown nail to develop. Some people also have nails that naturally grow in a curved or fan-like shape that can make ingrown nails more likely. If you have a painful or infected ingrown toenail, or if you are prone to ingrown toenails, it is suggested that you seek the care of a podiatrist.
An ingrown toenail occurs when the outer edge of a toenail grows into the surrounding skin, rather than over it. This causes redness, swelling, pain, and inflammation around the ingrown toenail. The area is also at an increased risk of infection. Several factors make an ingrown toenail more likely to develop. Trimming the toenails improperly, by cutting them too short or into a rounded shape, makes the skin more likely to fold over the nail. Wearing shoes that are too tight or narrow in the toe area can squish the nails into the skin. Having excessively sweaty feet can make the skin surrounding the nails too soft, allowing the nail to pierce through the skin more easily. Sometimes an injury to the toenail can cause an ingrown nail to develop. Some people also have nails that naturally grow in a curved or fan-like shape that can make ingrown nails more likely. If you have a painful or infected ingrown toenail, or if you are prone to ingrown toenails, it is suggested that you seek the care of a podiatrist.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact the podiatrists of Dr. Siegerman & Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
An ingrown toenail is a nail that has curved downward and grown into the skin. This typically occurs at either the nail borders or the sides of the nail. As a result, pain, redness, swelling, and warmth may occur in the toe. If a break in the skin forms due to the ingrown nail, bacteria may enter and cause an infection in the area; this is typically characterized by a foul odor and drainage.
Ingrown toenails have multiple reasons for developing. In many instances, the condition is a result of genetics and is inherited. The most common cause, however, is improper trimming; cutting the toenails too short forces the skin beside the nail to fold over. An ingrown toenail can also develop due to trauma, such as stubbing the toe, having an object fall on the toe, or participating in activities that involve repeated kicking or running. Wearing shoes that are too tight or too short can also cause ingrown toenails.
Treatment for an ingrown toenail varies between patients and the severity of the condition. In most cases, it is best to see your podiatrist for thorough and proper treatment. After examining your toe, your podiatrist may prescribe oral antibiotics to clear the infection if one is present. Surgical removal of either a portion of the nail or the entire nail may also be considered. In some cases, complete removal or destruction of the nail root may be required. Most patients who undergo nail surgery experience minimal pain afterward and can return to normal activity the following day.
Ingrown toenails can be prevented with proper nail trimming and by avoiding improper-fitting shoes. When cutting the toenails, be sure that you are cutting in a straight line and avoid cutting them too short. Shoes should not be too short or tight in the toe box.
One of the foot’s 26 bones is called the navicular bone, which sits just in front of the ankle on the top of your foot. A stress fracture of the navicular bone is commonly the result of explosive and repetitive action of the feet, especially during running fast or jumping. During activity, the navicular bone may be squeezed between the two bones in front of and in back of it, causing stress. Symptoms of a navicular stress fracture are an ache in the midfoot area, including the inside of the arch, and pain if you press on the bone. This discomfort may subside once activity is stopped and the foot rests, but is likely to recur when the action starts again. If you have pain when flexing your foot upward, you may have a navicular fracture. A visit to a podiatrist for diagnostic imaging tests is a good idea. Treatment options, depending on the severity of the injury, include a walking splint, a full cast, or surgery.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact the podiatrists from Dr. Siegerman & Associates. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Chronic venous insufficiency is a condition in which the walls and valves of veins in the lower limbs do not function properly. This causes excessive pooling of blood in the lower limbs, resulting in heaviness, tension, swelling, aching, and cramping in the lower legs. One way to diagnose chronic venous insufficiency is through a venous Doppler ultrasound, which uses sound waves to show what the blood flow in the lower legs looks like. Ultrasounds are fast, safe, painless, and provide a great deal of data to help your doctor determine the correct diagnosis and monitor the health of your lower limbs. For more information about chronic venous insufficiency, please consult with a podiatrist.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with the podiatrists from Dr. Siegerman & Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
Fungal infections of the toenail (onychomycosis) can cause nails to thicken, turn yellow, and possibly separate from the nail bed. Onychomycosis can be very stubborn and difficult to treat. This is because the nail grows so slowly, and fungus gets in between the multiple layers making up the nail, under the nail, or even in the nail matrix. Laser treatment for fungal nails is believed to be an effective and safe treatment for the eradication of onychomycosis. This is because the laser can penetrate the nail and be precisely targeted to attack the fungus without damaging surrounding skin or tissue. Laser treatment for fungal nails can take as little as one treatment and prevent the infection from spreading or returning. If you have developed a fungal toenail infection, ask your podiatrist if laser treatment is right for you.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with the podiatrists from Dr. Siegerman & Associates. Our doctors will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact one of our offices located in Drexel Hill and West Chester, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A new treatment for fungal nails, or onychomycosis, which has grown in popularity in recent years, is laser treatment. Laser treatment involves the use of a laser that kills fungus in the toenail with heat. Laser therapy causes no side effects and does not affect nearby healthy tissue.
Toenail fungus afflicts almost 10 percent of the U.S. population and is more common among the elderly. The most common symptom of toenail fungus is the discoloration and thickening of the nail. The nail can also become brittle and a foul smell may be produced. In rare cases, pain might be present. While it is not a serious condition, it can lead to a perception of disgust amongst those it affects. There are several different fungi that cause fungal infections. These include dermatophyte, yeast, and mold. The most common of these is dermatophyte.
Diagnosis for fungal nails involves a podiatrist utilizing microscopy and fungal cultures. This will allow the doctor to determine whether it is a fungus or another condition, such as lichen planus, psoriasis, nail damage, and onychogryphosis.
Fungus in the nails can be hard to get rid of with over-the-counter drugs. This is due to the nail being hard and protective, with fungus able to slip between the nail bed and plate. Furthermore the slow growth of the nail increases the difficulty of fungus going away. Laser treatment seeks to get around this by directly penetrating through the nail and killing the fungus. The laser is used on each infected nail for a couple of minutes. Patients then typically return several weeks or months later for another laser treatment. During this time the podiatrist will routinely observe the foot and infection. It is also recommended to wear clean socks and shoes and allow the feet to dry and breathe to prevent toenail fungus.
Laser treatment is still a relatively new treatment and not all podiatrists have laser machines. Ask your podiatrist if they do laser treatment for toenail fungus and if it is right for you.
Request a free copy of
Laser Away Foot Pain!
today.